Binge eating disorder is the most common eating disorder in the United States, affecting an estimated 2.8 million Americans at any given time. It is a serious mental health condition where a person repeatedly consumes large amounts of food in short periods while feeling a complete loss of control. Binge eating disorder causes are rooted in a complex mix of psychological, biological, and environmental factors that drive the behavior well beyond ordinary overeating.
This is not a willpower problem. It is a recognized DSM-5 diagnosis that requires professional evaluation and treatment. Understanding what causes binge eating disorder, how to recognize its symptoms, and what treatment options are available is the first step toward recovery.
Highlights
- Binge eating disorder (BED) is the most prevalent eating disorder in the U.S., affecting approximately 2.8 million people and occurring at nearly twice the combined rate of anorexia and bulimia nervosa combined (National Eating Disorders Association, 2023).
- The American Psychiatric Association formally recognized BED as a distinct DSM-5 diagnosis in 2013, separating it from the broader category of “eating disorder not otherwise specified.”
- Research consistently links binge eating disorder to co-occurring psychiatric conditions: 79% of people with BED have at least one lifetime psychiatric diagnosis, most commonly depression, anxiety, or PTSD (Hudson et al., 2007).
- Stress binge eating is one of the most documented triggers. Studies show elevated cortisol levels directly increase cravings for high-fat, high-sugar foods and impair the brain’s impulse control systems.
- Cognitive behavioral therapy (CBT) reduces binge eating frequency by 48 to 98% in clinical trials and is the most evidence-based treatment currently available for binge eating disorder.
What Is Binge Eating Disorder?
Binge eating disorder (BED) is a psychiatric condition characterized by recurrent episodes of eating unusually large amounts of food accompanied by a subjective sense of loss of control. Unlike bulimia nervosa, binge eating disorder does not involve regular compensatory behaviors such as purging, excessive exercise, or fasting after a binge episode. This distinction makes BED particularly dangerous because the physical consequences of repeated bingeing accumulate without any attempt at reversal.
The American Psychiatric Association included BED as a formal DSM-5 diagnosis in 2013. Before that, it was classified under the catch-all category of “eating disorder not otherwise specified.” Its formal recognition reflects decades of research establishing it as a distinct condition with a specific etiology, symptom profile, and treatment pathway.
DSM-5 Diagnostic Criteria for Binge Eating Disorder
To meet the DSM-5 clinical threshold for binge eating disorder, a person must experience recurrent binge episodes at least once per week for three months. A binge episode is defined as eating a distinctly large amount of food in a discrete period, accompanied by a sense of lack of control. During binge episodes, at least three of the following must be present:
- Eating much more rapidly than normal
- Eating until feeling uncomfortably full
- Eating large amounts of food when not physically hungry
- Eating alone because of embarrassment about how much one is eating
- Feeling disgusted, depressed, or guilty after overeating
The binge eating must cause marked distress and must not be associated with regular compensatory behaviors or occur exclusively during the course of bulimia nervosa or anorexia nervosa.
BED is classified by severity based on binge frequency per week: mild (1 to 3 episodes), moderate (4 to 7 episodes), severe (8 to 13 episodes), and extreme (14 or more episodes).
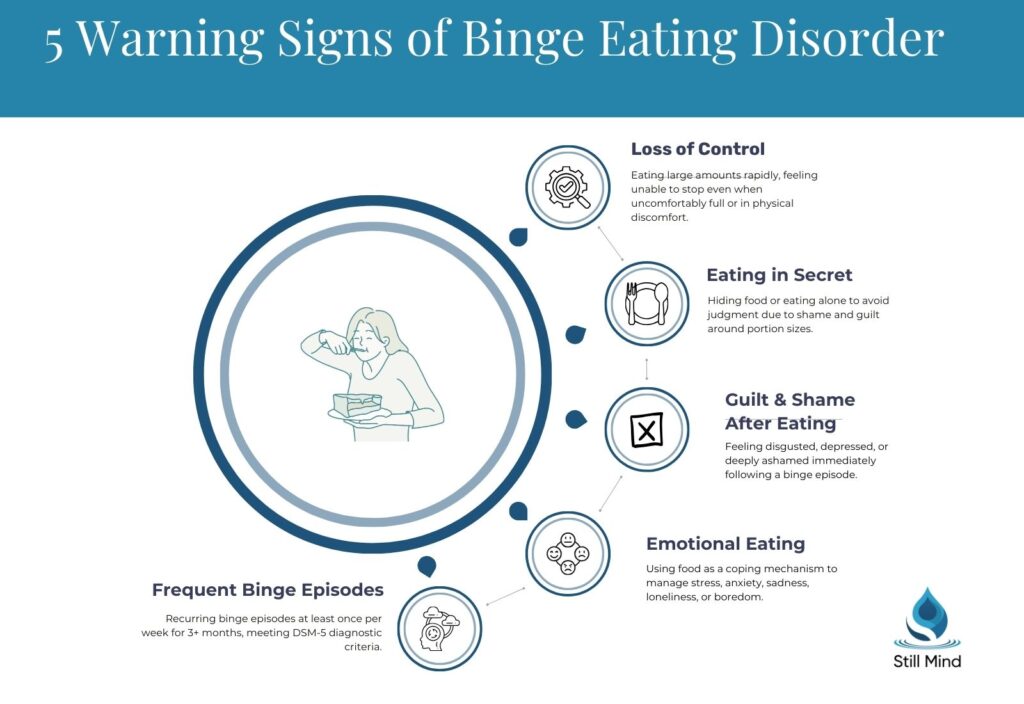
Symptoms of Binge Eating Disorder
Binge eating disorder symptoms span behavioral, emotional, and physical domains. They are not always visible to others, as many people with BED eat normally around others and binge only in private.
Behavioral Symptoms
- Eating large quantities of food in a short time, often within two hours
- Continuing to eat well past physical fullness or discomfort
- Eating in secret or hiding food for later consumption
- Hoarding food or stockpiling specific binge foods
- Frequently starting restrictive diets but abandoning them quickly
- Organizing the day around binge episodes, including planning and protecting time for them
Emotional Symptoms
- Feeling a loss of control during a binge that feels impossible to stop
- Intense guilt, shame, or disgust immediately after bingeing
- Using food to cope with negative emotions including stress, sadness, loneliness, and boredom
- Feeling emotionally numb or dissociated during a binge episode
- Persistent preoccupation with food, weight, and body image
- Chronic low self-esteem connected to eating behavior and body shape
Physical Symptoms and Health Risks
- Significant weight fluctuations over time
- Gastrointestinal distress including bloating, acid reflux, and abdominal discomfort
- Fatigue, disrupted sleep, and poor energy related to erratic eating patterns
- Development of obesity-related health conditions including type 2 diabetes, hypertension, and cardiovascular disease
Binge Eating at Night
Nighttime binge eating is one of the most commonly reported patterns in people with BED. As daily structure and distractions dissolve in the evening, emotional triggers like loneliness, stress, and fatigue become more prominent. Restrictive eating during the day also plays a direct role. When the body and mind have been denied adequate food earlier, the evening hours produce intense urges that override impulse control. This restriction and binge cycle is one of the most self-sustaining patterns in the disorder.
What Causes Binge Eating Disorder?
Binge eating disorder causes are multifactorial. No single factor creates the disorder on its own. Research consistently points to an interaction between biological vulnerability, psychological patterns, and environmental exposures that together create the conditions for BED to develop and persist.
Psychological Causes of Binge Eating Disorder
Psychological factors are among the most well-documented causes of binge eating disorder. Negative emotions serve as the most common direct trigger for binge episodes. People with BED typically use food as an emotional regulation tool, turning to binge eating to temporarily reduce anxiety, loneliness, shame, or emotional numbness.
Low self-esteem, chronic dissatisfaction with body image, perfectionism, and difficulty tolerating negative emotional states all increase vulnerability. Research consistently shows that binge eating disorder and depression are closely linked, with depression and BED frequently occurring together and each worsening the other when left untreated.
People with emotional dysregulation are at particular risk. When the brain lacks effective tools for managing distress, food becomes a fast and reliably accessible source of temporary emotional relief. This is not a conscious choice. It is a pattern wired through repeated learning and neurological reinforcement.
Biological and Genetic Causes
Genetics play a meaningful role in binge eating disorder. Studies of twins suggest that BED has a heritability rate of approximately 41 to 57%, meaning genetic factors explain a significant portion of individual risk. A family history of eating disorders, mood disorders, or substance use disorders all increase vulnerability.
At the neurobiological level, dysregulation of the dopamine reward system is a primary driver. Binge eating triggers a surge in dopamine that creates a powerful reinforcement loop, making the behavior feel compulsive and difficult to interrupt. Research also identifies serotonin dysregulation as contributing to impaired impulse control and appetite regulation in people with BED.
Elevated cortisol from chronic stress directly increases appetite for calorie-dense foods and impairs the prefrontal cortex’s ability to override impulsive eating decisions. This is why stress binge eating has such strong neurobiological underpinnings and is not simply a behavioral choice.
Trauma and Adverse Childhood Experiences
Childhood trauma is one of the strongest and most consistently identified causes of binge eating disorder. Childhood emotional neglect, physical or sexual abuse, chronic household stress, and bullying, particularly weight-related bullying, all significantly elevate BED risk.
Trauma disrupts the development of healthy emotional regulation skills and creates associations between food and psychological safety. When a child learns that eating soothes distress, that neural pathway strengthens over years of repetition into a default coping mechanism that is extraordinarily difficult to interrupt in adulthood without professional support.
History of Dieting and Restrictive Eating
Paradoxically, repeated cycles of restrictive dieting are a significant cause of binge eating disorder. Chronic dietary restriction creates physiological deprivation and psychological preoccupation with forbidden foods. When restriction eventually breaks, the resulting binge is both physiologically driven and psychologically intensified by the guilt and shame that follow the “failure” to maintain the diet.
This restriction and binge cycle is self-reinforcing. Each completed cycle strengthens the association between rigid control and eventual loss of control, embedding BED deeper into a person’s relationship with food.
Environmental and Social Factors
Societal and cultural pressure to achieve a specific body type creates chronic body dissatisfaction that is one of the strongest environmental risk factors for all eating disorders. Social media exposure to unrealistic body ideals has been shown to increase eating disorder risk, particularly in adolescents and young adults.
Family environment also contributes. Growing up in households where food was used as reward or punishment, where critical comments about weight were routine, or where dieting was modeled as normal behavior all increase the likelihood of developing a disordered relationship with food.
Mental Health Conditions Associated With Binge Eating Disorder
Binge eating disorder rarely occurs in isolation. Understanding co-occurring conditions is critical for building an effective treatment plan.
| Co-Occurring Condition | How It Connects to Binge Eating Disorder |
|---|---|
| Major Depression | Negative mood states are the most common immediate trigger for binge episodes |
| Anxiety Disorders | Anxiety drives emotional eating as avoidance; food temporarily dampens anxious arousal |
| PTSD | Binge eating develops as a dissociative coping response to traumatic memories and hyperarousal |
| Borderline Personality Disorder (BPD) | Emotional dysregulation and identity disturbance fuel compulsive eating as an emotion regulation tool |
| Bipolar Disorder | Hypomanic and depressive phases both independently increase binge eating risk |
| ADHD | Impulsivity and poor inhibitory control reduce ability to interrupt binge episodes once initiated |
| OCD | Food-related obsessions and compulsive eating rituals share overlapping neurological pathways |
| Substance Use Disorders | Shared reward system dysregulation and impulse control deficits create dual vulnerability |
The connection between borderline personality disorder and binge eating is particularly well-documented. BPD involves intense emotional dysregulation and a chronic sense of emptiness, and binge eating frequently serves as a primary coping mechanism for both. People with bipolar disorder also experience elevated rates of BED, with binge episodes occurring during both depressive lows and hypomanic periods driven by impulsivity and reduced inhibition.
Risks and Complications of Binge Eating Disorder
Without treatment, binge eating disorder carries significant physical and psychological health risks that compound over time.
Physical health risks include:
- Obesity and significant weight gain over time
- Type 2 diabetes and insulin resistance
- Cardiovascular disease including hypertension and elevated cholesterol
- Sleep apnea and chronic sleep disruption
- Gastrointestinal complications including acid reflux and irritable bowel syndrome
- Chronic pain conditions associated with inflammation and excess weight
Psychological and functional risks include:
- Deepening depression, shame, and social withdrawal
- Progressive deterioration of occupational and social functioning
- Development or worsening of co-occurring anxiety and mood disorders
- Increased risk of suicidal ideation, particularly when BED co-occurs with depression or trauma
Research published in the Harvard Gazette (2024) found that BED is both more widespread and more persistent than previously understood, with many cases going undiagnosed for years due to stigma and misdiagnosis.
Treatment for Binge Eating Disorder
Binge eating disorder is highly treatable. The most effective approaches combine psychotherapy, medication where appropriate, nutritional support, and treatment of co-occurring mental health conditions.
Cognitive Behavioral Therapy (CBT)
CBT is the most evidence-based treatment for binge eating disorder. It directly targets the distorted thoughts and maladaptive behaviors that maintain the binge cycle. Clinical trials consistently show CBT reduces binge frequency by 48 to 98%. CBT for BED focuses on identifying emotional triggers for bingeing, challenging all-or-nothing thinking about food and body image, building distress tolerance skills, and establishing structured, regular eating patterns that break the restriction and binge cycle.
Dialectical Behavior Therapy (DBT)
DBT is particularly effective for people with BED who also struggle with emotional dysregulation, trauma, or BPD. DBT’s core skill sets, including mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness, directly address the emotional triggers and coping deficits that drive binge eating. Research supports DBT as one of the most effective treatments for binge eating in populations with complex psychiatric histories.
Medication for Binge Eating Disorder
The only FDA-approved medication for binge eating disorder is lisdexamfetamine (Vyvanse), a stimulant medication originally developed for ADHD that has been shown in clinical trials to significantly reduce binge frequency. It is typically reserved for moderate to severe cases.
SSRIs including sertraline and fluoxetine are commonly prescribed off-label to address the depression and anxiety that co-occur with BED and contribute to binge triggers. Topiramate, an anticonvulsant, has also demonstrated efficacy in reducing binge episodes in controlled trials. Medication should always be used alongside psychotherapy rather than as a standalone intervention.
Nutritional Counseling
Working with a registered dietitian who specializes in eating disorders helps people with BED restore a regular, structured relationship with food. Nutritional counseling addresses physiological deprivation patterns, dismantles the restrictive eating that fuels binges, and helps rebuild neutral, non-judgmental attitudes toward food. This component is essential for addressing the physical side of recovery alongside the psychological work in therapy.
Treating Co-Occurring Conditions
Because the majority of people with BED have at least one co-occurring psychiatric diagnosis, effective treatment must address those underlying conditions simultaneously. Untreated anxiety or depression will continue to generate the emotional distress that drives binge episodes even when behavioral interventions are partially effective. Integrated treatment that targets both BED and its co-occurring conditions produces substantially better outcomes than treating each in isolation.
Frequently Asked Questions
What is the best treatment for binge eating disorder?
Cognitive behavioral therapy (CBT) is currently the most evidence-based treatment for binge eating disorder and is recommended as the first-line intervention by major clinical guidelines. DBT is highly effective for people with significant emotional dysregulation. Lisdexamfetamine (Vyvanse) is the only FDA-approved medication for BED and may be appropriate for moderate to severe cases. The most effective outcomes come from combining therapy, nutritional counseling, and treatment of any co-occurring mental health conditions.
What is an example of a binge eat?
A typical example is consuming an entire bag of chips, multiple portions of leftovers, and a box of cookies within 30 to 45 minutes while alone in the evening, then feeling intensely ashamed and physically uncomfortable afterward. The person feels unable to stop once the episode starts, despite wanting to. The food consumed is usually significantly more than most people would eat in that time under similar circumstances. The sense of loss of control during the episode is the defining feature.
What medication is used for binge eating?
Lisdexamfetamine (Vyvanse) is the only medication with FDA approval specifically for moderate to severe binge eating disorder. SSRIs including fluoxetine and sertraline are widely prescribed off-label to address co-occurring depression and anxiety. Topiramate has shown efficacy in clinical trials for reducing binge frequency. All medication for BED should be managed by a psychiatrist in conjunction with ongoing psychotherapy and nutritional support.
What are the risks of binge eating disorder?
Physical risks include obesity, type 2 diabetes, cardiovascular disease, sleep apnea, and gastrointestinal complications. Psychological risks include worsening depression, deepening shame and social isolation, progressive functional impairment, and increased risk of suicidal ideation when BED co-occurs with mood disorders or trauma. Without treatment, BED tends to become more entrenched over time rather than resolving on its own. Early professional intervention significantly improves long-term outcomes.
References
- American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5th ed.). American Psychiatric Publishing.
- Hudson, J. I., Hiripi, E., Pope, H. G., and Kessler, R. C. (2007). The prevalence and correlates of eating disorders in the National Comorbidity Survey Replication. Biological Psychiatry, 61(3), 348-358.
- National Eating Disorders Association. (2023). Binge eating disorder.
- National Institute of Mental Health. (2023). Eating disorders. https://www.nimh.nih.gov/health/topics/eating-disorders
- Centers for Disease Control and Prevention. (2023). Adult obesity facts. https://www.cdc.gov/obesity/data/adult.html
- Grilo, C. M., and Mitchell, J. E. (Eds.). (2010). The treatment of eating disorders: A clinical handbook. Guilford Press.
- Reas, D. L., and Grilo, C. M. (2015). Pharmacological treatment of binge eating disorder. International Journal of Eating Disorders, 48(7), 869-875.
- Striegel-Moore, R. H., and Franko, D. L. (2008). Should binge eating disorder be included in the DSM-5? International Journal of Eating Disorders, 41(8), 649-660.






