Hallucinations are false sensory perceptions that feel completely real.
They occur without any external stimulus, yet the brain registers them with the same intensity as genuine sight, sound, smell, taste, or touch.
Most people associate hallucinations exclusively with psychiatric illness. In reality, they arise from dozens of causes, including neurological conditions, substance withdrawal, severe sleep deprivation, high fever, and medication side effects.
Understanding what causes a hallucination determines how it is treated. A visual hallucination in a person with Parkinson’s disease requires a completely different clinical response than an auditory hallucination in someone with schizophrenia or an olfactory hallucination following a temporal lobe seizure.
Key Takeaways
- According to epidemiological research published in peer-reviewed literature, an estimated 6 to 15 percent of the general population experiences hallucinations at some point during their lifetime, with sleep-related hallucinations occurring in up to 70 percent of people.
- Auditory hallucinations are the most clinically significant type, present in the majority of people diagnosed with schizophrenia spectrum disorders, and are the primary symptom driving psychiatric hospitalization.
- The National Institute of Mental Health reports that schizophrenia, the mental health condition most closely associated with hallucinations, affects between 0.25 and 0.64 percent of U.S. adults.
- According to PMC research, 25 to 30 percent of auditory hallucinations in schizophrenia remain refractory to traditional antipsychotic medications, requiring augmented treatment approaches.
What Are Hallucinations?
A hallucination is a sensory experience that arises entirely from within the brain rather than from an external source, distinguishing it clinically from both an illusion and a delusion.
Hallucination vs. Illusion vs. Delusion
These three terms are frequently confused, but each describes a distinct neurological or psychological phenomenon with different diagnostic implications.
Clinical distinctions between the three:
- Hallucination: A sensory perception that occurs with no external stimulus present, experienced as fully real by the individual at the time of occurrence, regardless of insight.
- Illusion: A misinterpretation of a stimulus that actually exists, such as mistaking a shadow for a figure or hearing one’s name in ambient noise.
- Delusion: A fixed false belief rather than a false sensory experience, such as the conviction that others are plotting against the individual despite evidence to the contrary.
Pseudohallucinations and Insight
A pseudohallucination is a sensory experience that resembles a hallucination but occurs alongside intact insight, meaning the individual recognizes the experience as internally generated rather than externally real.
Key clinical distinction:
- Psychotic hallucinations: Occur without insight. The individual believes the perception is real and external, which classifies the experience as a positive symptom of psychosis within DSM-5-TR diagnostic criteria.
- Pseudohallucinations with intact insight: Include the vivid visual experiences of Charles Bonnet syndrome and the hypnagogic imagery that occurs as a person falls asleep. These are neurological phenomena rather than psychiatric symptoms.

How Hallucinations Form in the Brain
Hallucinations arise when the brain’s sensory processing systems generate perceptual signals without receiving input from the external environment, through mechanisms that vary depending on the underlying cause.
Dopaminergic Pathway Dysregulation
Mesolimbic dopamine hyperactivity generates aberrant salience, assigning emotional significance to internally generated neural noise and producing the perception that the signal has an external source.
The dopamine mechanism in psychiatric hallucinations:
- Excessive mesolimbic dopaminergic transmission: Dopamine D2 receptor overstimulation in the mesolimbic pathway drives the hallucinations associated with schizophrenia spectrum disorders, producing primarily auditory hallucinations involving voices that comment on or issue commands to the individual.
- Antipsychotic mechanism: Second-generation antipsychotics reduce hallucination frequency and intensity by blocking mesolimbic D2 receptors, directly interrupting the aberrant salience signal generation that makes internally produced perceptions feel externally real.
Sensory Deprivation and Cortical Hyperactivity
When sensory organs stop transmitting adequate input to the brain’s processing regions, those cortical areas become hyperactive and begin generating their own perceptual signals to compensate for the missing data.
The sensory deprivation mechanism:
- Charles Bonnet syndrome: Visual cortex hyperactivity in response to macular degeneration, glaucoma, or retinitis pigmentosa produces vivid, detailed visual hallucinations of people, animals, geometric patterns, and objects. The brain fills in the missing visual data with internally generated imagery, analogous to phantom limb sensations following amputation.
- Musical ear syndrome: Auditory hallucinations in individuals with significant hearing loss follow the same cortical compensation mechanism, producing persistent musical or voice-like sounds in the absence of any external auditory input.
Neurochemical Disruption from Substances
Psychoactive substances produce hallucinations by directly disrupting the neurochemical balance of serotonin, dopamine, glutamate, and endocannabinoid systems that regulate normal sensory processing.
Substance-specific mechanisms:
- Classic psychedelics (LSD, psilocybin): 5-HT2A serotonin receptor agonism in the visual cortex and prefrontal cortex produces intense visual distortions and full hallucinations by flooding serotonergic pathways beyond their normal perceptual filtering capacity.
- Stimulants (methamphetamine, cocaine): Dramatic elevation of mesolimbic dopamine through reuptake inhibition and release produces paranoid auditory hallucinations, particularly following prolonged use or binge patterns that exhaust presynaptic dopamine stores.
- Alcohol withdrawal: Sudden cessation of alcohol in dependent individuals triggers GABA-A receptor hyperactivity and glutamate rebound, producing the vivid tactile and visual hallucinations of delirium tremens during severe alcohol withdrawal.
The 5 Types of Hallucinations
Hallucinations are classified by the sensory modality in which they occur, each type reflecting distinct underlying neurobiological mechanisms and associating with different clinical conditions.
1- Auditory Hallucinations
Auditory hallucinations are the most clinically prevalent type, defined as hearing sounds, voices, music, or environmental noises without any external acoustic source.
Clinical features of auditory hallucinations:
- Command auditory hallucinations: Voices that issue direct instructions represent the most clinically dangerous subtype, as they carry elevated risk of self-harm or harm to others and are a primary indicator for inpatient psychiatric assessment.
- Commentary auditory hallucinations: Voices that narrate, critique, or comment on the individual’s actions in real time are among the most diagnostically significant positive symptoms of schizophrenia spectrum disorders in the DSM-5-TR.
- Referential auditory hallucinations: Hearing one’s own thoughts spoken aloud, or voices conversing about the individual in the third person, represent the Schneiderian first-rank symptom historically considered pathognomonic of schizophrenia.
2- Visual Hallucinations
Visual hallucinations involve seeing objects, people, animals, lights, or geometric patterns that have no external physical presence, and are most commonly associated with neurological rather than purely psychiatric conditions.
Clinical associations of visual hallucinations:
- Parkinson’s disease: Visual hallucinations occur in up to 50 percent of people with Parkinson’s disease as the condition progresses, often presenting as well-formed human or animal figures and frequently associated with dopaminergic medication effects.
- Lewy body dementia: Recurrent, detailed visual hallucinations are one of the earliest and most diagnostically characteristic features of Lewy body dementia, often appearing before significant cognitive decline.
- Psychotic break in schizophrenia: Visual hallucinations in schizophrenia spectrum disorders tend to involve distorted human figures, body parts, or unrecognizable objects rather than the well-formed scenes more typical of neurological causes.
3- Olfactory Hallucinations
Olfactory hallucinations are perceived smells without an external odor source, most commonly described as burning, chemical, or rotting odors.
Clinical associations:
- Temporal lobe epilepsy: Seizures originating in or near the piriform cortex and uncus produce brief, stereotyped olfactory hallucinations as part of an ictal aura, often preceding the tonic-clonic phase.
- Brain tumors and lesions: Tumors in the temporal or frontal lobe can generate persistent or episodic olfactory hallucinations that reflect direct cortical irritation rather than psychiatric pathology.
4- Tactile Hallucinations
Tactile hallucinations involve the perception of physical sensations on or within the body without any external physical contact.
Clinical associations:
- Cocaine and stimulant use disorder: Formication, the tactile hallucination of insects crawling on or under the skin, is a well-documented symptom of cocaine use disorder and stimulant use disorder, particularly during prolonged use or acute stimulant toxicity.
- Alcohol withdrawal and delirium tremens: Severe alcohol withdrawal produces tactile hallucinations of insects, burning sensations, or the feeling of being touched, occurring alongside the visual hallucinations and autonomic instability of delirium tremens.
5- Hypnagogic and Hypnopompic Hallucinations
Hypnagogic hallucinations occur at sleep onset and hypnopompic hallucinations occur upon waking, representing an intermediate neurological state between dreaming and full wakefulness.
Clinical features:
- Normal occurrence: Sleep-related hallucinations are experienced by up to 70 percent of people at some point during their lives and are classified as benign neurological phenomena rather than psychiatric symptoms when they occur in the absence of other pathology.
- Incubus experience: The perception of a menacing presence combined with sleep paralysis, with a lifetime prevalence of approximately 30 percent, represents a specific hypnopompic hallucination type driven by incomplete REM sleep transition rather than psychosis.

What Causes Hallucinations?
Hallucinations arise from psychiatric conditions, neurological disorders, substance use, medical conditions, and situational triggers, each producing hallucinations through distinct mechanisms that require different clinical responses.
Psychiatric Causes
Psychiatric conditions produce hallucinations by disrupting the neurochemical systems that regulate sensory reality testing, most commonly through dopaminergic and serotonergic pathway dysregulation.
Psychiatric conditions that cause hallucinations:
- Schizophrenia spectrum disorders: Schizophrenia, schizoaffective disorder, schizophreniform disorder, brief psychotic disorder, and delusional disorder all generate hallucinations as core positive symptoms through mesolimbic dopamine hyperactivity.
- Bipolar disorder with psychotic features: Bipolar disorder with psychotic features produces hallucinations during severe manic or depressive episodes, most frequently auditory and typically mood-congruent in content.
- Post-traumatic stress disorder: Post-traumatic stress disorder generates trauma-related perceptual re-experiencing, including auditory and tactile hallucinations that replay sensory elements of the traumatic event.
Neurological Causes
Neurological conditions produce hallucinations through cortical hyperactivity, seizure activity, neurotransmitter depletion, or structural changes that disrupt the brain’s normal sensory filtering mechanisms.
Neurological conditions that cause hallucinations:
- Parkinson’s disease: Dopamine depletion in the nigrostriatal pathway combined with dopaminergic medication effects produces visual hallucinations in up to half of people with advanced Parkinson’s disease.
- Temporal lobe epilepsy: Ictal discharges in the temporal lobe generate stereotyped auditory, olfactory, or gustatory hallucinations as part of a seizure aura, distinguishable from psychiatric hallucinations by their brief, repetitive, and predictable nature.
- Alzheimer’s disease and dementia: Advanced Alzheimer’s disease most commonly produces visual hallucinations, while Lewy body dementia generates early, recurrent, and highly detailed visual hallucinations as one of its core diagnostic features.
Substance-Related Causes
Substance intoxication and withdrawal both generate hallucinations through opposing neurochemical mechanisms, making the substance use history a critical component of hallucination assessment.
Substance causes of hallucinations:
- Alcohol withdrawal delirium tremens: Sudden cessation of heavy, long-term alcohol use triggers severe GABA rebound and glutamate hyperactivity, producing vivid tactile and visual hallucinations that represent a medical emergency requiring immediate clinical management.
- Psychedelic hallucinogens: LSD, psilocybin, mescaline, DMT, and salvia produce hallucinations by directly binding to and overstimulating 5-HT2A serotonin receptors in the visual and prefrontal cortex, generating perceptual distortions that resolve as the substance is metabolized.
- Hallucinogen persisting perception disorder (HPPD): A subset of individuals who use psychedelic hallucinogens develop HPPD, a condition in which visual disturbances and perceptual alterations persist long after the substance has cleared the system.
Medical and Situational Causes
Medical conditions and situational triggers generate hallucinations through physiological disruption of normal brain chemistry without the sustained neurological or psychiatric pathology of chronic conditions.
Medical and situational causes:
- High fever and severe infection: Febrile hallucinations result from inflammatory cytokine effects on the blood-brain barrier and neurotransmitter function, most commonly producing visual hallucinations that resolve when the underlying infection is treated.
- Severe sleep deprivation: Progressive sleep deprivation disrupts the REM-waking boundary, generating visual and auditory hallucinations after approximately 72 hours of continuous wakefulness, resolving fully with adequate restorative sleep.
- Sensory deprivation: Prolonged deprivation of visual or auditory input triggers cortical hyperactivity in the deprived sensory modality, generating hallucinations within as few as 15 minutes of complete sensory isolation in susceptible individuals.
How to Stop Hallucinations: Treatment and Management
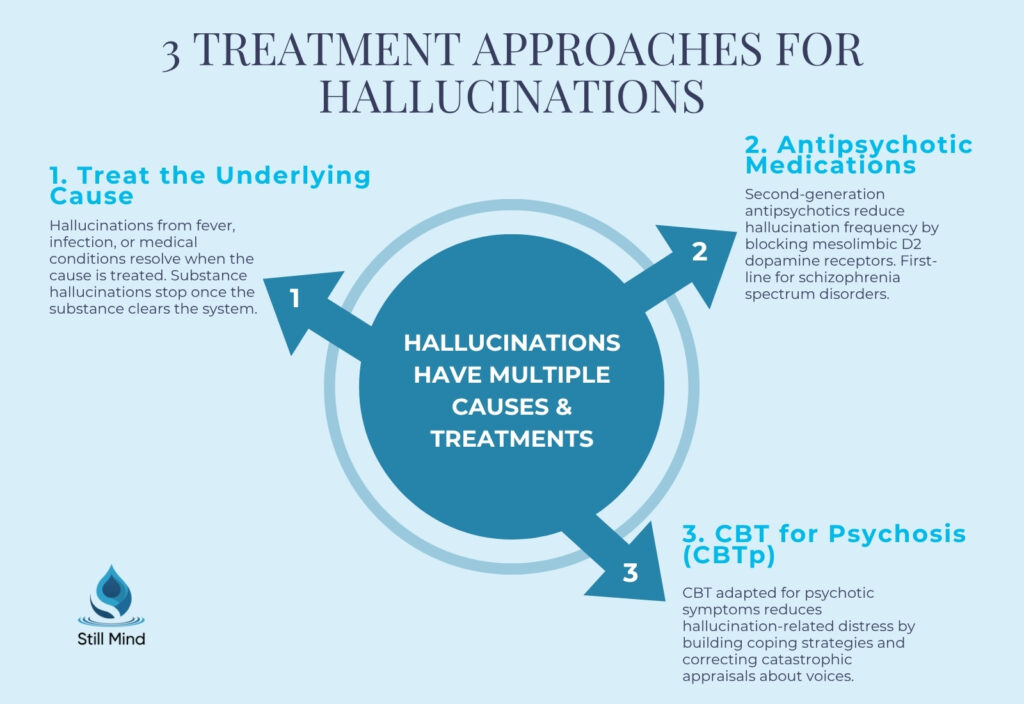
Treatment for hallucinations targets the underlying cause rather than the hallucination itself, as the appropriate intervention varies completely depending on whether the origin is psychiatric, neurological, substance-related, or situational.
Medication Approaches
Pharmacological treatments by cause:
- Antipsychotic medications for psychiatric hallucinations: Second-generation antipsychotics including risperidone, olanzapine, quetiapine, and aripiprazole reduce auditory and visual hallucinations in schizophrenia spectrum disorders by blocking mesolimbic D2 dopamine receptors. Clozapine remains the evidence-based option for treatment-resistant hallucinations that do not respond to two adequate antipsychotic trials.
- Parkinson’s disease-specific treatment: Standard antipsychotics worsen Parkinson’s motor symptoms by blocking nigrostriatal dopamine receptors, requiring the use of clozapine at low doses or pimavanserin, an atypical antipsychotic that targets 5-HT2A receptors without affecting dopamine.
- Medical condition management: Hallucinations caused by fever, infection, or metabolic disturbance resolve when the underlying medical condition is adequately treated, without requiring antipsychotic medication.
Therapy and Non-Pharmacological Approaches
Evidence-based psychological approaches:
- CBT for psychosis (CBTp): Cognitive behavioral therapy adapted for psychotic symptoms reduces hallucination-related distress without necessarily eliminating the hallucinations, helping individuals evaluate the meaning, source, and urgency of voices and build behavioral coping strategies.
- Hallucination-focused integrative treatment (HIT): This structured 20-session approach integrates CBT, psychoeducation, coping skills training, and medication management over 9 to 12 months, showing effectiveness for chronic schizophrenia and psychotic adolescents with persistent auditory hallucinations.
- Charles Bonnet syndrome reassurance: The most critical intervention for Charles Bonnet syndrome is psychoeducation confirming that the visual hallucinations result from vision loss rather than psychiatric illness, as many individuals fear they are losing their minds and experience significant relief from understanding the neurological mechanism.
Mental Health Treatment at Still Mind Florida
Still Mind Florida provides structured outpatient mental health care for adults experiencing hallucinations associated with psychotic disorders, mood disorders, trauma, and anxiety conditions.
Psychoeducation for Psychotic Symptoms
Psychoeducation at Still Mind Florida covers:
- Comprehensive education about hallucination types, triggers, and neurobiological mechanisms, supporting individuals in recognizing their symptom patterns and developing informed strategies for daily management.
- Family-focused sessions that build caregiver knowledge of hallucination warning signs, crisis recognition, and effective communication strategies with loved ones experiencing perceptual disturbances.
Evidence-Based Outpatient Care
Outpatient clinical services include:
- Individualized treatment planning aligned with DSM-5-TR diagnostic criteria for schizophrenia spectrum disorders, bipolar disorder with psychotic features, and PTSD-related perceptual experiences.
- Clinical assessments for individuals seeking evaluation of new or worsening hallucinations are available, with same-day intake scheduling for acute presentations.
Frequently Asked Questions
What is the most common cause of hallucinations?
The most common cause of clinically significant hallucinations is schizophrenia spectrum disorder, particularly schizophrenia itself. Auditory hallucinations involving voices are the most prevalent symptom. However, hallucinations overall are most frequently caused by benign neurological events, including sleep-related hypnagogic and hypnopompic experiences, which affect up to 70 percent of people.
What are the 5 types of hallucinations?
The five primary types are auditory (hearing sounds or voices), visual (seeing objects or figures), olfactory (perceiving phantom smells), tactile (feeling sensations on or under the skin), and hypnagogic or hypnopompic hallucinations that occur at sleep onset or waking. Gustatory hallucinations, involving phantom tastes, are a sixth less common type.
How do you stop hallucinations?
Treatment depends entirely on the cause. Psychiatric hallucinations are treated with antipsychotic medications and CBT for psychosis. Hallucinations from fever or infection resolve when the medical condition is treated. Substance-related hallucinations typically stop once the substance clears the system. Sleep deprivation hallucinations resolve with adequate rest.
What is the first stage of hallucination?
In psychiatric contexts, the first stage typically involves heightened internal perceptual sensitivity, where internal neural noise becomes increasingly difficult to distinguish from external stimuli. This prodromal state precedes the full auditory hallucinations of established psychosis. In substance-induced contexts, the first stage involves perceptual distortions such as visual trailing, color intensification, or pattern movement before full hallucinations emerge.
References
- National Institute of Mental Health. (2024). Schizophrenia. U.S. Department of Health and Human Services. https://www.nimh.nih.gov/health/topics/schizophrenia
- Badcock, J. C., Dehon, H., & Laroi, F. (2017). Hallucinations in healthy aging. Frontiers in Aging Neuroscience. https://pmc.ncbi.nlm.nih.gov/articles/PMC3105559/
- Substance Abuse and Mental Health Services Administration. (2023). Key substance use and mental health indicators. https://www.samhsa.gov/data/report/2023-nsduh-annual-national-report
- American Psychiatric Association. (2022). Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision (DSM-5-TR). American Psychiatric Publishing.
- Cleveland Clinic. (2022). Hallucinations: Definition, causes, treatment and types. Cleveland Clinic Medical.
- National Institute of Neurological Disorders and Stroke. (2024). Parkinson’s disease information. https://www.ninds.nih.gov/health-information/disorders/parkinsons-disease
- Mayo Clinic. (2024). Hallucinations: Symptoms and causes. Mayo Foundation for Medical Education and Research.






