Ketamine therapy for depression has moved from experimental curiosity to a clinically recognized treatment option over the past two decades. For people with treatment-resistant depression who have not responded to antidepressants, it offers a mechanism of action that is fundamentally different from anything available before. Understanding how ketamine works for depression, what the real risks are, and whether it is appropriate for your situation is essential before pursuing this path.
This guide covers everything you need to know: the science, the types of treatment, the side effects, and the questions most people have before their first session.
Highlights
- Ketamine produces measurable antidepressant effects within hours of a single infusion, compared to two to six weeks for traditional antidepressants, according to research published in the National Institute of Mental Health (NIMH, 2006).
- The FDA approved esketamine (Spravato) nasal spray in 2019 specifically for treatment-resistant depression and major depressive disorder with acute suicidal ideation, making it the first genuinely new class of antidepressant approved in over 30 years.
- A 2022 Columbia University study published in Cell Reports found that repeated ketamine use produces structural changes in the brain’s dopamine system, with implications for cognition and long-term psychological health.
- Studies show that up to 30% of heavy recreational ketamine users develop some form of urinary tract dysfunction, including ketamine-induced ulcerative cystitis (NIH, 2022).
- Research from the National Institute on Drug Abuse (NIDA) indicates that approximately half of people living with a mental illness will also develop a substance use disorder, making careful patient selection critical before ketamine treatment begins.
What Is Ketamine Therapy for Depression?
Ketamine therapy for depression involves the controlled, medically supervised administration of ketamine to reduce depressive symptoms, particularly in people who have not responded to conventional antidepressant medications. First synthesized in 1962 and approved by the FDA in 1970 as an anesthetic, ketamine was recognized as a rapid-acting antidepressant following a landmark 2006 NIMH study showing that a single intravenous dose produced significant antidepressant effects within hours.
It is classified as a Schedule III controlled substance in the United States, legal for use in licensed medical settings but illegal for recreational possession or distribution outside of them.
Ketamine is sometimes called a “dirty drug” in pharmacological literature because it acts on multiple neural pathways simultaneously rather than targeting a single receptor system. This broad mechanism explains both its clinical effectiveness and its range of risks.
How Does Ketamine Work for Depression?
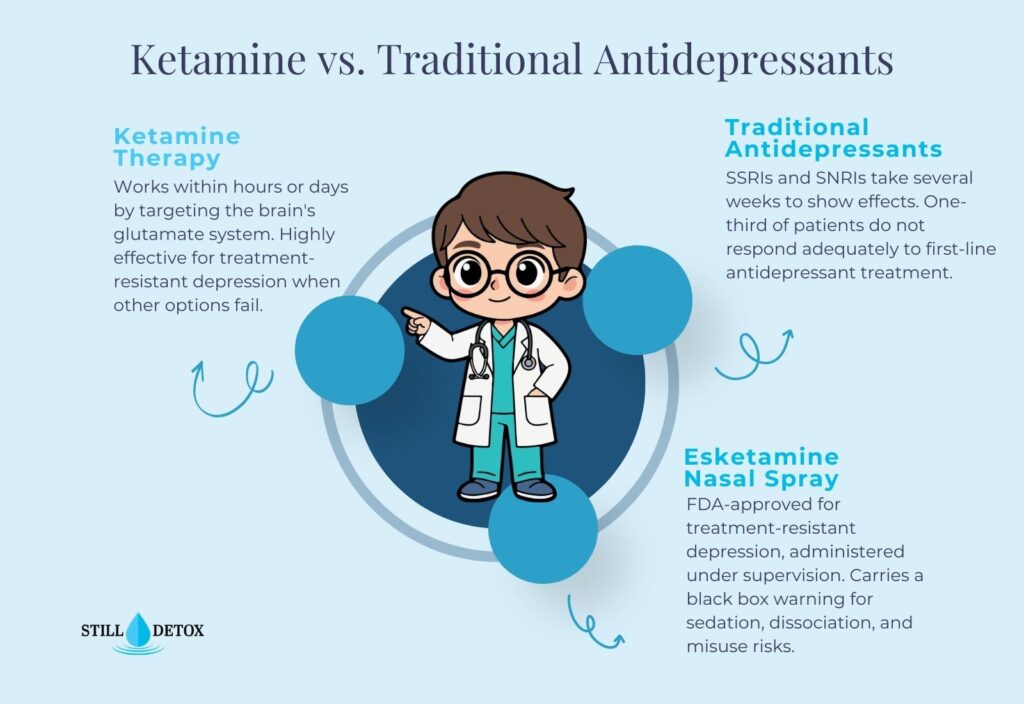
Traditional antidepressants such as SSRIs primarily target the serotonin system and require weeks of daily dosing to produce effects. Ketamine works differently and much faster. Its primary mechanism targets the glutamate system, the brain’s most abundant excitatory neurotransmitter.
Ketamine blocks NMDA receptors, which are glutamate receptors involved in synaptic plasticity, learning, and emotional regulation. This blockade triggers a rapid surge in AMPA receptor activity, which researchers believe promotes neuroplasticity, the brain’s ability to form new neural connections. In people with depression, this process appears to rapidly restore disrupted neural circuits in the prefrontal cortex and hippocampus, areas governing mood, executive function, and emotional processing.
In simpler terms: ketamine essentially jump-starts synaptic communication in regions of the brain that depression has suppressed, often producing relief within hours rather than weeks.
How Does Ketamine Help With Anxiety and PTSD?
The same glutamatergic mechanism that helps with depression also appears beneficial for anxiety disorders and PTSD. In PTSD, ketamine may help interrupt the reconsolidation of fear memories by disrupting NMDA-dependent memory processes during treatment sessions. Research is still emerging, but several controlled trials have shown measurable reductions in PTSD symptom severity following ketamine infusion.
Types of Ketamine Treatment for Depression
Not all ketamine delivery methods are equivalent. The administration route significantly affects bioavailability, onset, duration, and risk profile.
| Type | Administration | FDA Status | Setting | Notes |
|---|---|---|---|---|
| IV Ketamine Infusion | Intravenous drip | Off-label for depression | Clinic only | Highest bioavailability; most studied form |
| Esketamine (Spravato) | Nasal spray | FDA-approved (2019) | In-clinic, supervised | S-enantiomer of ketamine; patient self-administers under observation |
| IM Ketamine | Intramuscular injection | Off-label | Clinic only | Less precise dosing than IV |
| Oral/Sublingual Ketamine | Tablet or troche | Off-label | At-home with telehealth supervision | Lower bioavailability; less predictable effects |
| At-Home Compounded Ketamine | Oral tablet via telehealth | Off-label; FDA warning issued | At-home | FDA warns patients may not receive adequate risk information |
The FDA issued a formal warning about compounded ketamine products prescribed through telehealth platforms, citing concern that patients may not receive critical safety information about the risks associated with unsupervised use at home. IV infusion in a licensed clinical setting remains the gold standard for ketamine therapy for depression.
Does Ketamine Therapy Work for Depression?
The clinical evidence is meaningful, particularly for treatment-resistant depression. A significant proportion of patients with depression that has not responded to two or more antidepressant medications show a rapid and substantial response to ketamine infusion. Some studies report response rates of 50 to 70% in this population following a standard course of six infusions over two to three weeks.
However, several important caveats apply.
Ketamine’s antidepressant effects are typically temporary without ongoing maintenance treatment. Most patients experience relief for days to weeks after a single infusion. Sustained benefits generally require repeated sessions and, in many cases, integration with ongoing psychotherapy to address the root psychological patterns driving the depression.
It is not a cure. It is a tool, and its effectiveness depends heavily on patient selection, clinical setting, dosing protocol, and what support structures are in place after treatment ends.
How Many Ketamine Treatments Are Needed for Depression?
A standard initial course of ketamine therapy for depression typically involves six IV infusions administered over two to three weeks, usually every two to three days. This protocol is based on early clinical trial designs and remains the most widely used approach.
After the initial series, some patients require monthly or quarterly maintenance infusions to sustain the antidepressant benefit. Others experience longer-lasting relief and may not need maintenance sessions for several months. Individual response varies considerably, and the appropriate schedule is determined in consultation with the treating psychiatrist.
Esketamine (Spravato) follows a different protocol: twice weekly for four weeks during the induction phase, then weekly for four weeks, followed by weekly or every-two-week maintenance dosing depending on response.
How Long Does Ketamine Work for Depression?
The duration of benefit is one of the most significant limitations of ketamine therapy. Following a single infusion, antidepressant effects can last anywhere from a few days to several weeks depending on the individual. After a full initial course of six infusions, many patients sustain benefit for four to six weeks. Some report longer periods.
For long-term management, ketamine is most effectively combined with evidence-based psychotherapy such as cognitive behavioral therapy. The neuroplasticity window opened by ketamine may enhance responsiveness to therapeutic work during the period immediately following treatment, making the post-infusion period an important opportunity for psychological integration.
Short-Term Side Effects of Ketamine Therapy
Side effects during and immediately after a ketamine infusion are common but generally time-limited. Most resolve within one to two hours of treatment completion. Patients are always monitored on-site during infusions for this reason.
Common short-term side effects include:
- Dissociation or feeling detached from your surroundings
- Perceptual distortions, visual or sensory
- Dizziness, nausea, or vomiting
- Elevated heart rate and blood pressure
- Blurred vision
- Mild confusion or disorientation immediately post-infusion
- Drowsiness or fatigue lasting several hours after treatment
- Temporary anxiety or agitation during the infusion itself
The dissociative experience during treatment is expected and is not considered a medical emergency in a supervised setting. It typically resolves fully within one to two hours. Patients are advised not to drive on the day of treatment.
Long-Term Side Effects of Ketamine for Depression
Long-term side effects are the most clinically important consideration for anyone weighing ketamine therapy. These risks are primarily associated with chronic, high-dose use and are more pronounced in recreational contexts. However, they are not irrelevant for people undergoing repeated therapeutic infusions over months or years.
Cognitive and Psychological Effects
Chronic ketamine use, particularly at recreational doses, has been associated with memory impairment, reduced attention span, difficulty with complex cognitive tasks, and persistent brain fog. A study published in the Journal of Psychopharmacology found that heavy, long-term users showed significant impairments in working memory, verbal memory, and executive function.
Persistent dissociation is another concern. Some individuals who use ketamine repeatedly, particularly recreationally, report experiencing dissociative states even when not under the drug’s influence. People who already live with derealization or depersonalization disorder may be at higher risk for this complication and should discuss this with their prescribing clinician before pursuing ketamine treatment.
Structural Brain Changes
A 2022 Columbia University study published in Cell Reports found that extended, repeated ketamine use produces widespread structural changes in the dopamine system. These findings raise important questions about the long-term neurological implications of ongoing maintenance ketamine therapy, particularly for younger patients whose brains remain more plastic.
Physical Side Effects
Long-term physical side effects include damage to nasal and sinus cavities in people who snort ketamine recreationally, vein and tissue damage in intravenous users, and cardiovascular strain including elevated blood pressure, increased heart rate, and respiratory complications in high-risk patients.
The most serious physical complication of chronic use is ketamine-induced ulcerative cystitis, also known as ketamine bladder syndrome. Studies show that up to 30% of heavy ketamine users develop some form of urinary tract dysfunction, ranging from frequent urination and bladder pain to severe structural bladder damage requiring surgical intervention. This risk is primarily associated with recreational use but has been reported in therapeutic contexts involving frequent dosing.
Risk of Dependence and Addiction
Ketamine carries a risk of psychological dependence. This is especially relevant for people with a personal or family history of substance use disorders, or for individuals with dual diagnosis presentations where a mental health condition co-occurs with a substance use disorder. Research from NIDA indicates that approximately half of people with a mental illness will also develop a substance use disorder at some point in their lives, making careful pre-treatment screening essential.
Chronic users of ketamine, according to published research, tend to show higher rates of depression than occasional users, meaning that unsupervised or excessive use can paradoxically worsen the condition it is meant to treat.
Ketamine Therapy vs. Recreational Use: Key Differences
The risks associated with ketamine are not equivalent across all use contexts. Administration route, dose, frequency, and clinical oversight are the critical variables that separate therapeutic benefit from harm.
| Factor | Medical/Therapeutic Use | Recreational Use |
|---|---|---|
| Administration | IV infusion or supervised nasal spray | Snorting, oral, or injection without supervision |
| Dose | Carefully calculated sub-anesthetic dose | Variable; often higher to achieve desired effect |
| Bioavailability control | Precise | Inconsistent and unpredictable |
| Monitoring | Continuous on-site clinical monitoring | None |
| Frequency | Structured protocol with clinical review | Uncontrolled, often escalating |
| Addiction risk | Present but mitigated by supervision | Significantly higher |
| Dissociation management | Managed in safe clinical environment | Unmanaged; K-hole risk |
| Long-term safety oversight | Ongoing clinical assessment | Absent |
The K-hole, a state of intense dissociation associated with very high doses, is a risk specific to recreational use where dosing is uncontrolled. In clinical settings, doses are kept at sub-anesthetic levels that produce therapeutic effects without reaching this level of disconnection from reality.
Who Should Not Receive Ketamine Therapy?
Ketamine therapy is not appropriate for everyone. Clinicians use comprehensive pre-treatment screening to assess individual suitability. People with the following conditions or histories are typically considered poor candidates:
- Active psychosis or a history of psychotic disorders such as schizophrenia or schizoaffective disorder
- Uncontrolled hypertension or significant cardiovascular disease
- A personal history of ketamine misuse or current substance use disorder
- Active mania or hypomanic episodes in bipolar disorder without adequate mood stabilization
- Pregnancy
- Severe liver disease
- A strong personal or family history of dissociative disorders
People with extreme mood swings that have not been properly diagnosed should receive a thorough psychiatric evaluation before ketamine is considered, as treating an undiagnosed bipolar disorder with ketamine without mood stabilization can destabilize mood further.
Ketamine Therapy in Florida
Ketamine therapy is legally available across Florida through licensed psychiatric and medical providers. Clinics offering IV ketamine infusions and esketamine (Spravato) administration operate in Fort Lauderdale, Boca Raton, and throughout the South Florida region. Patients seeking ketamine treatment in Fort Lauderdale or ketamine therapy in Boca Raton should work with board-certified psychiatrists who conduct full mental health evaluations before initiating treatment.
At Still Mind Florida, we provide comprehensive psychiatric assessment and evidence-based treatment for depression, treatment-resistant mood disorders, and co-occurring mental health conditions for patients across South Florida and nationwide. If you are considering ketamine therapy or need support navigating your treatment options, our team can help you determine the right path forward.
Frequently Asked Questions
How does ketamine work for depression?
Ketamine blocks NMDA receptors in the glutamate system, triggering a surge in neuroplasticity that restores disrupted neural circuits in areas of the brain governing mood and executive function. This mechanism is fundamentally different from SSRIs and produces antidepressant effects within hours rather than weeks. It is particularly effective for treatment-resistant depression where conventional antidepressants have failed to produce an adequate response.
How long does ketamine work for depression?
The antidepressant effects of a single ketamine infusion typically last from a few days to several weeks depending on individual response. A full initial course of six infusions can extend benefits to four to six weeks or longer. Most patients require some form of maintenance treatment and benefit most when ketamine is combined with ongoing psychotherapy to address underlying psychological patterns.
Does ketamine therapy get you high?
Ketamine at therapeutic doses produces dissociative and perceptual effects during the infusion that some patients describe as unusual or dream-like. These effects are expected and are not the same as a recreational high. They are managed in a clinical setting and resolve within one to two hours. The goal of therapeutic dosing is to reach levels that promote neuroplasticity without inducing the intense dissociation associated with recreational misuse.
What are the side effects of ketamine treatment for depression?
Short-term side effects during treatment include dissociation, dizziness, nausea, elevated blood pressure and heart rate, and temporary perceptual changes. These resolve within hours. Long-term risks from repeated use include cognitive impairment, persistent dissociation, structural brain changes, bladder dysfunction, and psychological dependence. Long-term risks are most pronounced in high-dose recreational contexts but are a real clinical consideration for patients pursuing ongoing maintenance infusions.
Is ketamine therapy legal in Florida?
Yes. Ketamine is a Schedule III controlled substance in the United States and is legal for use in licensed medical settings including ketamine infusion clinics and psychiatric practices. FDA-approved esketamine (Spravato) nasal spray can also be legally prescribed for treatment-resistant depression and administered in certified healthcare settings across Florida. Recreational possession or distribution of ketamine outside of medical contexts remains illegal.
References
- National Institute of Mental Health. (2006). Single dose of ketamine rapidly reduces depression. https://www.nimh.nih.gov
- U.S. Food and Drug Administration. (2019). FDA approves new nasal spray medication for treatment-resistant depression. https://www.fda.gov/news-events/press-announcements/fda-approves-new-nasal-spray-medication-treatment-resistant-depression
- U.S. Food and Drug Administration. (2023). FDA warns patients and health care providers about potential risks associated with compounded ketamine products. https://www.fda.gov/drugs/human-drug-compounding/fda-warns-patients-and-health-care-providers-about-potential-risks-associated-compounded-ketamine
- National Institutes of Health. (2022). Urinary tract dysfunction in ketamine users. PLOS ONE. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9476224/
- National Institutes of Health. (2021). Cognitive impairments associated with long-term ketamine use. National Library of Medicine. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8972190/
- Bhatt, D. L., et al. (2022). Dopamine system structural changes with repeated ketamine use. Cell Reports, Columbia University.
- National Institute on Drug Abuse. Comorbidity: Substance use disorders and other mental illnesses. https://nida.nih.gov/research-topics/comorbidity
- Drug Enforcement Administration. (2023). Drug scheduling. https://www.dea.gov/drug-scheduling






