ADHD paralysis is a state of mental overwhelm where individuals with ADHD become unable to initiate, continue, or complete tasks despite genuinely wanting to do so.
Unlike simple procrastination or laziness, this neurobiological phenomenon stems from executive dysfunction in the prefrontal cortex, where dopamine regulation issues and working memory deficits create a literal cognitive freeze.
The National Institute of Mental Health recognizes executive dysfunction as one of the core impairments in ADHD, affecting millions of children and adults in the United States. So why does an ADHD brain freeze at the exact moment you need it to work, and what does it take to break free from this neurological gridlock?
Key Takeaways
- ADHD paralysis occurs when executive dysfunction in the prefrontal cortex prevents task initiation despite conscious intention to act, distinguishing it from procrastination or motivational issues.
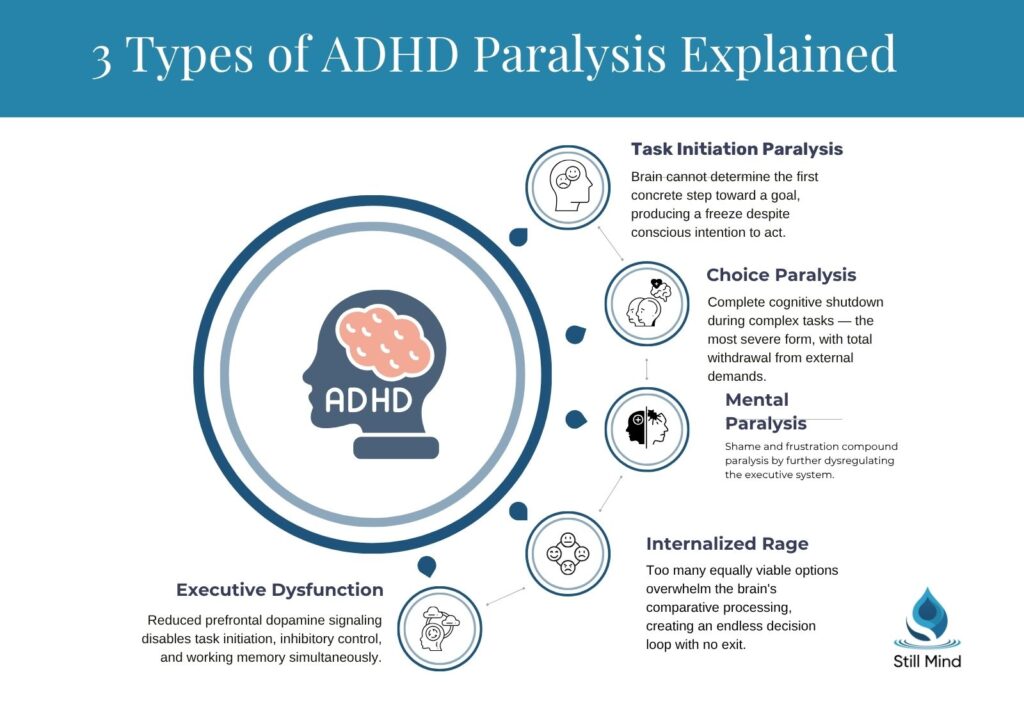
- The three primary types include task initiation paralysis (inability to start), choice paralysis (overwhelm from too many options), and mental paralysis (complete cognitive shutdown during complex thinking).
- The Substance Abuse and Mental Health Services Administration emphasizes that executive function impairments significantly impact daily functioning and require targeted intervention strategies rather than traditional productivity advice.
- Brain imaging reveals reduced activation in the anterior cingulate cortex and altered default mode network connectivity during paralysis episodes, explaining why willpower alone cannot overcome these episodes.
- Evidence-based interventions focus on dopamine priming, environmental modifications, and body doubling techniques that work with ADHD neurobiology rather than against it, with professional treatment recommended when paralysis interferes with basic activities of daily living.
What Is ADHD Paralysis and Why Does It Happen?
ADHD paralysis represents a fundamental breakdown in the brain’s executive control systems.
The prefrontal cortex, which manages working memory, cognitive flexibility, and inhibitory control, becomes overwhelmed and essentially shuts down its task-initiation functions. This neurobiological event differs dramatically from typical procrastination because the individual experiences a genuine inability to act, not unwillingness. The brain’s dopamine pathways, already dysregulated in ADHD, fail to provide the neurochemical fuel needed for task engagement. Meanwhile, the anterior cingulate cortex, responsible for effort allocation and conflict monitoring, shows reduced activation during these episodes.
Russell Barkley, a leading ADHD researcher, describes executive dysfunction as the brain’s “CEO going offline.” When paralysis strikes, individuals report feeling mentally trapped while watching themselves fail to perform even simple actions.
The cascade typically begins with cognitive overload. Multiple competing demands, unclear task parameters, or decision fatigue overwhelm the brain’s limited executive resources. This triggers a protective shutdown that paradoxically makes the situation worse by preventing any forward progress. The emotional toll compounds the problem, as shame and frustration further dysregulate an already struggling system.
The Three Types of ADHD Paralysis
ADHD paralysis manifests in three distinct patterns, each with unique triggers and characteristics. Understanding these differences helps identify targeted intervention strategies.
| Paralysis Type | Primary Trigger | Duration Pattern | Cognitive Experience | Best Intervention |
|---|---|---|---|---|
| Task Initiation | Unclear starting point | Minutes to hours | Blank staring, physical frozenness | Micro-commitments, body doubling |
| Choice Paralysis | Too many options | Extended periods | Analysis loops, decision avoidance | Option elimination, time limits |
| Mental Paralysis | Complex cognitive demands | Hours to days | Brain fog, complete shutdown | Cognitive rest, environmental reduction |
Task initiation paralysis occurs when the brain cannot determine the first concrete step toward a goal.
Even simple tasks like washing dishes become impossible because the executive system fails to break the activity into actionable components. The individual knows what needs to happen but cannot translate that knowledge into the first physical action.
Choice paralysis emerges from decision fatigue when too many equally viable options overwhelm the brain’s comparative processing abilities. The American Psychiatric Association notes that individuals with ADHD often struggle with decision-making due to working memory limitations that prevent them from holding multiple options in mind simultaneously. This creates a loop where each option consideration erases the previous one, making comparison impossible.
Mental paralysis represents the most severe form, involving complete cognitive shutdown during intellectually demanding activities.
What Does ADHD Paralysis Feel Like From the Inside?
The subjective experience of ADHD paralysis combines physical, emotional, and cognitive components that create a distinctly recognizable pattern.
Individuals describe feeling “trapped in amber” or “watching themselves from outside their body” as their brain refuses to engage with necessary tasks. Physically, paralysis episodes often include muscle tension, particularly in the shoulders and jaw, combined with a heavy, lethargic sensation throughout the body. Many report feeling simultaneously wired and exhausted, as if their nervous system is stuck between activation and shutdown.
The eyes may fixate on the task or screen without processing information, creating a blank staring state.
Emotionally, shame and self-criticism intensify the experience. Individuals berate themselves for not “just doing it,” which creates additional stress that further impairs executive function. This emotional layer distinguishes ADHD paralysis from anhedonia, where people lose interest in activities rather than wanting to act but being unable to do so. Cognitively, racing thoughts compete with mental fog in a paradoxical combination.
Why Traditional Productivity Advice Fails for ADHD Paralysis
Standard productivity strategies often backfire for individuals experiencing ADHD paralysis because they assume a neurotypical executive function baseline.
“Just start” or “break it into smaller pieces” advice can intensify paralysis by adding additional cognitive demands to an already overwhelmed system. The ADHD brain operates with different dopamine regulation patterns, requiring intrinsic motivation and interest to fuel task engagement. Traditional time management focuses on external structure and discipline, which bypasses the neurochemical processes that actually drive ADHD task initiation. Breaking tasks into smaller components can worsen choice paralysis by multiplying decision points.
When executive function is already compromised, creating more steps often increases overwhelm rather than reducing it.
Willpower-based approaches prove particularly counterproductive because they rely on the exact executive functions that paralysis has disabled. Telling someone in ADHD paralysis to “just focus” is equivalent to telling someone with a broken leg to “just walk”: the underlying system necessary for the action is temporarily non-functional. Similarly, prioritization strategies fail because the paralyzed brain cannot engage in the comparative analysis that prioritization requires.
How to Recognize ADHD Paralysis: A Symptom Assessment
ADHD paralysis exists on a severity spectrum from mild episodes that resolve within hours to severe presentations requiring professional intervention.
Mild ADHD Paralysis (Self-Management Appropriate)
- Duration: 30 minutes to 4 hours per episode
- Frequency: A few times per week
- Impact: Delays completion of non-urgent tasks
- Recovery: Responds to environmental changes or mild stimulation
- Functioning: Maintains basic activities of daily living
Moderate ADHD Paralysis (Consider Professional Support)
- Duration: 4-24 hours per episode
- Frequency: Daily or multiple times daily
- Impact: Interferes with work, school, or relationship responsibilities
- Recovery: Requires significant intervention or external assistance
- Functioning: Inconsistent self-care and social engagement
Severe ADHD Paralysis (Immediate Professional Intervention)
- Duration: Days to weeks of persistent paralysis
- Frequency: Nearly constant state
- Impact: Complete inability to perform essential tasks
- Recovery: Does not respond to self-help strategies
- Functioning: Impaired basic self-care and safety
Evidence-Based Strategies to Break ADHD Paralysis
Effective paralysis intervention works with ADHD neurobiology rather than against it, focusing on dopamine regulation, cognitive load reduction, and executive function support.
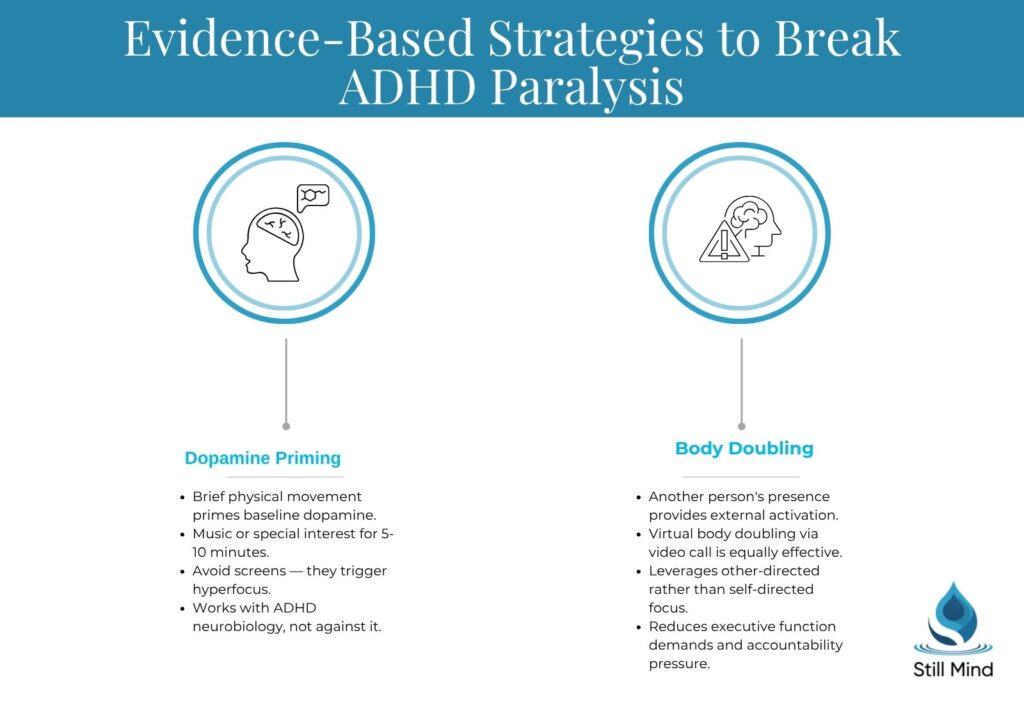
Dopamine Priming Techniques
The ADHD brain requires adequate dopamine to initiate and sustain task engagement.
Dopamine priming involves deliberately engaging in brief, enjoyable activities that boost baseline dopamine before attempting challenging tasks. Effective dopamine primers include physical movement, music, brief social interaction, or engaging with a special interest for 5-10 minutes. The key is choosing activities that reliably generate positive feelings without becoming hyperfocused time sinks.
Avoid using screens or social media as dopamine primers, as these can trigger hyperfocus states that worsen paralysis by further depleting executive resources.
Body Doubling and External Activation
Body doubling leverages the ADHD brain’s responsiveness to external stimulation and social presence. Having another person present, either physically or virtually, provides the external activation energy that paralyzed executive function cannot generate internally. The body double doesn’t need to assist with the task directly, their mere presence helps regulate attention and provides subtle accountability pressure. Virtual body doubling through video calls or co-working sessions can be equally effective for remote work or study situations.
This strategy works because ADHD brains often struggle with self-directed attention but respond well to other-directed or externally cued attention.
Environmental Modifications for Reduced Cognitive Load
Environmental changes can dramatically reduce the cognitive demands that trigger and maintain paralysis states.
These modifications focus on eliminating decision points, reducing visual distractions, and creating clear action pathways. Remove visual clutter from the immediate task environment to reduce competing attention demands. Pre-organize materials and tools so task initiation requires minimal executive planning. Create physical or visual cues that prompt the next action step without requiring memory or decision-making.
Single-tasking environments prove particularly crucial, as task-switching demands can immediately trigger new paralysis episodes in vulnerable individuals.
The ADHD-Modified 2-Minute Rule
Traditional productivity advice suggests doing any task that takes less than two minutes immediately.
For ADHD paralysis, this approach requires modification because time estimation is often impaired and the “immediate action” component can trigger executive dysfunction. The ADHD version focuses on committing to just two minutes of engagement with a task, regardless of completion. This micro-commitment reduces the psychological pressure that often maintains paralysis while creating momentum through action initiation. Set a visible timer and agree to stop after two minutes if desired.
Often, task engagement naturally continues once the initial paralysis breaks, but the permission to stop prevents the overwhelm that keeps individuals frozen.
When Does ADHD Paralysis Require Professional Treatment?
Professional intervention becomes necessary when ADHD paralysis significantly impairs basic functioning or persists despite consistent self-management efforts.
Paralysis episodes lasting longer than one week suggest possible co-occurring conditions such as depression, anxiety disorders, or trauma-related responses that require specialized treatment. The combination of ADHD and other mental health conditions creates complex interactions that self-help strategies cannot adequately address. When paralysis interferes with basic activities of daily living (eating, sleeping, personal hygiene, or safety behaviors), immediate professional intervention is crucial.
The American Academy of Child and Adolescent Psychiatry recommends professional evaluation when executive dysfunction symptoms significantly impact academic, occupational, or social functioning for extended periods.
The Role of Medication in Managing ADHD Paralysis
Stimulant and non-stimulant medications can significantly improve executive function and reduce paralysis frequency by addressing underlying dopamine regulation issues.
However, medication alone rarely eliminates paralysis episodes completely without accompanying behavioral strategies. Stimulant medications like methylphenidate and amphetamines enhance prefrontal cortex function and improve task initiation abilities. Non-stimulant options such as atomoxetine may benefit individuals who cannot tolerate stimulants or have co-occurring anxiety that stimulants worsen. Medication timing becomes crucial for paralysis management, as many individuals experience “rebound” periods when medication effects wane.
Working with prescribers to optimize timing and duration helps maintain consistent executive function throughout demanding parts of the day.
The Neurobiology of ADHD Paralysis: What Brain Imaging Reveals
Recent brain imaging studies illuminate the specific brain activity patterns that occur during ADHD paralysis episodes, revealing why these experiences feel so distinctly different from typical procrastination or avoidance behaviors.
Functional magnetic resonance imaging shows reduced activation in the anterior cingulate cortex during paralysis states, explaining why individuals lose the ability to monitor their performance or adjust their approach when stuck. This brain region normally helps evaluate effort demands and decide whether to persist with or abandon tasks. The default mode network, active during rest and internal focus, shows altered connectivity patterns in ADHD paralysis. Instead of properly deactivating during task-focused periods, these networks remain highly active, creating competing internal chatter that interferes with external task engagement.
This explains the subjective experience of racing thoughts combined with inability to act.

Treatment for ADHD and Executive Dysfunction
Comprehensive treatment for ADHD paralysis addresses both the underlying attention regulation difficulties and the specific executive dysfunction patterns that create paralysis episodes.
ADHD Treatment Programs
Specialized ADHD treatment programs provide comprehensive assessment and intervention for complex presentations involving severe executive dysfunction. These programs typically include neuropsychological testing to identify specific cognitive strengths and weaknesses, medication optimization, and intensive behavioral skill training focused on executive function development.
Cognitive Behavioral Therapy for ADHD
Cognitive Behavioral Therapy adapted for ADHD addresses the thought patterns and behavioral cycles that maintain paralysis states. CBT helps individuals recognize paralysis triggers, develop personalized intervention strategies, and address the shame and self-criticism that often worsen executive dysfunction episodes.
Dual Diagnosis Treatment
Many individuals with severe ADHD paralysis benefit from dual diagnosis treatment that addresses co-occurring mental health conditions such as anxiety, depression, or trauma responses.
The Bottom Line
ADHD paralysis is a neurobiological phenomenon that requires targeted interventions addressing dopamine regulation and executive dysfunction rather than traditional productivity approaches. Professional evaluation becomes crucial when paralysis episodes persist longer than one week or interfere with basic functioning, as this often indicates co-occurring conditions requiring specialized mental health treatment.
If you recognize persistent patterns of ADHD paralysis that interfere with your daily functioning, professional evaluation can help identify the most effective treatment approach for your specific needs and circumstances.
Frequently Asked Questions
What is an ADHD shutdown?
ADHD shutdown is an extreme form of paralysis where the brain completely disengages from external demands due to overwhelming sensory input, emotional stress, or cognitive overload. Unlike paralysis focused on specific tasks, shutdown involves complete withdrawal from social interaction, decision-making, and even basic self-care activities. This protective mechanism can last hours to days and typically requires significant rest and environmental reduction to resolve. Recovery often involves gradually reintroducing simple activities while maintaining reduced sensory and cognitive demands.
Can you have ADHD paralysis without having ADHD?
Task paralysis can occur in other conditions including anxiety disorders, depression, autism spectrum disorders, and during periods of extreme stress or burnout. However, the specific pattern of executive dysfunction combined with dopamine regulation issues creates a distinct presentation in ADHD that differs from paralysis in other conditions. ADHD paralysis typically involves the inability to initiate tasks despite wanting to complete them, while paralysis from anxiety often involves fear-based avoidance. Professional evaluation helps distinguish between ADHD-related paralysis and similar symptoms from other causes.
What is the developmental delay rule for ADHD?
The developmental delay rule suggests that individuals with ADHD typically function at developmental levels significantly behind their chronological age in areas of executive functioning and emotional regulation. This means a young adult with ADHD might have executive skills similar to someone much younger, which explains why age-typical expectations for task management and emotional control often feel overwhelming and can trigger paralysis episodes. Understanding this developmental gap helps set realistic expectations and choose age-appropriate interventions for executive skill building.
How long does ADHD paralysis typically last?
Mild paralysis episodes usually resolve within 30 minutes to 4 hours with appropriate intervention or environmental changes. Moderate episodes can persist for 4-24 hours and may require external support or significant strategy implementation to break. Severe paralysis lasting days to weeks typically indicates co-occurring mental health conditions requiring professional treatment. The duration often depends on the underlying triggers, available coping strategies, and whether the individual can access environmental modifications or external support during the episode.
Is ADHD paralysis the same as executive dysfunction?
ADHD paralysis is a specific manifestation of executive dysfunction, but executive dysfunction encompasses a broader range of difficulties including working memory problems, cognitive flexibility issues, and inhibitory control challenges. Paralysis specifically refers to the inability to initiate or continue tasks despite conscious intention, while executive dysfunction includes various cognitive control difficulties that may not necessarily prevent action. Someone might experience working memory deficits without paralysis, or have paralysis episodes while maintaining other executive functions. Both require different intervention approaches.
Can ADHD paralysis happen even with medication?
Individuals taking ADHD medications can still experience paralysis episodes, particularly during medication transition periods, times of high stress, or when facing especially complex or emotionally charged tasks. Medication improves baseline executive function but doesn’t eliminate all paralysis triggers, especially those related to perfectionism, overwhelm, or co-occurring mental health conditions. Combining medication with behavioral strategies typically provides better paralysis prevention than medication alone. Some people also experience rebound paralysis as medication effects wear off, requiring timing adjustments.
References
- American Academy of Child and Adolescent Psychiatry. (2024). Professional evaluation guidelines for executive dysfunction. https://www.aacap.org
- American Psychiatric Association. (2024). Decision-making and working memory limitations in ADHD.
- Barkley, R. (2024). Executive dysfunction as the brain’s CEO going offline.
- National Institute of Mental Health. (2024). Executive dysfunction as core impairment in ADHD. https://www.nimh.nih.gov
- Substance Abuse and Mental Health Services Administration. (2024). Executive function impairments and daily functioning intervention strategies. https://www.samhsa.gov






